What is Keratoconus and how is it treated?

Normal Shaped Cornea

Keratoconus Cornea
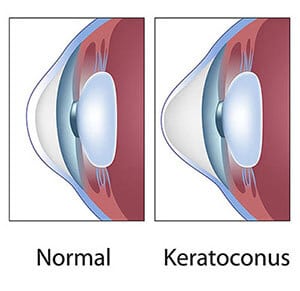
Keratoconus is a hereditary condition in which the cornea becomes thin and misshaped. Keratoconus often causes corneal scarring and severe astigmatism. Although glasses are sometimes enough to correct the vision of someone with keratoconus, more often keratoconus patients require rigid contact lenses and/or surgery to get adequate vision. There are many types of corneal surgery for keratoconus including: lamellar keratoplasty (LKP, ALK, DALK), penetrating keratoplasty (PKP), intacts, and collagen cross-linking. Soft contact lenses usually do not provide adequate visual correction in keratoconus patients.
What can I do to make keratoconus better?
Unfortunately, there are no dietary or lifestyle changes that will make keratoconus better. We do know that eye rubbing or other pressure on the eyes can stimulate progression of keratoconus. Wearing rigid contact lenses does not prevent the progression of the shape changes in keratoconus. Reading and normal use of the eyes does not make keratoconus worse. If necessary, the vision in an eye with keratoconus can be improved with a corneal transplant.
Can corneal collagen cross-linking help keratoconus?



Corneal Collagen + Vitamin B2 + Ultraviolet A light = Corneal Collagen Cross Linking
The cornea is made up of clear layers of collagen. These layers are connected together or “linked” by proteins. Their arrangement provides for the clarity and strength of the cornea. Keratoconus causes a breakdown of this collagen. Aggressive eye rubbing and time can contribute to this breakdown. Corneal collagen cross linking is an in office procedure that increases the links between the collagen. Thus, strengthening the cornea and helping to prevent the progression of keratoconus. The procedure can be done by removing the corneal surface (epi-off) or leaving the corneal surface in place (epi-on). Riboflavin (vitamin B2) drops are administered and then the cornea is exposed to an ultraviolet light for a short time. A bandage soft contact lens is placed on the eye for comfort at the end of the procedure and the patient goes home the same day using eye drops.
Keep in mind that the purpose of corneal collagen cross linking is not to make the vision clear on its own. The main goal of cross linking is to slow or stop steepening of the cornea and progression of keratoconus. Patients will often still need rigid contact lenses to get their best vision after cross linking. These are normally fitted approximately one month after cross linking. The best keratoconus specialist in Houston can help with the diagnosis and treatment of this condition.
Learn about Avedro KXL Corneal Cross-Linking!



If I have keratoconus, what are the chances that my children or other family members also have or will develop keratoconus?
Genetic testing is now available to help determine if you or your family members have genes connected with keratoconus. This testing is now available in Dr. Vital’s office. Research is ongoing.
Can someone have keratoconus in only one eye?
Keratoconus is a bilateral disease and is always considered to be present in both eyes even if only one eye is showing the characteristics. It is not uncommon for keratoconus to be much more severe in one eye than the other.
When is a corneal transplant needed for keratoconus?
When glasses are not providing good vision, and rigid contact lenses either are not comfortable, do not fit, will not stay in place, or are not providing good vision, corneal transplant surgery should be considered. Additionally, immediately prior to or after severe scarring or hydrops from keratoconus, corneal transplantation may be necessary. Some patients can go their entire life with keratoconus and never need surgery. Others may need surgery at a very young age.