Corneal Infections and Scars
How will a corneal scar affect my vision?
Corneal scars can have widely differing affects on vision. How the scar will affect vision depends on the location, size, depth, transparency, and surface smoothness of the scar. Some corneal scars do not affect vision at all. Some corneal scars cause vision problems only in certain lighting conditions or during certain activities such as driving at night. The first steps in evaluating the effects of a cornea scar include determining the cause and the activity of the scar. It is very difficult to predict the effects of a scar that is active and changing. For the vision in an eye with a corneal scar that is quiet, the vision should be corrected with glasses if possible. If glasses do not provide adequate vision, then a rigid contact lens is tried. If the contact does not provide adequate vision, the next step is a consideration of corneal surgery. This surgery could be a scraping of the surface of the cornea, or a corneal transplant. 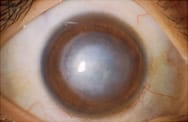
What are corneal infections or corneal ulcers?
Corneal infections have names such as infectious keratitis, corneal ulcers, and corneal infiltrates. These infections can be due to bacteria, viruses, or parasites. Corneal infections tend to be very painful and are often characterized by a red eye, sensitivity to light, and blurred vision. Improper contact lens care or excessive contact lens wearing is often the cause of infectious keratitis. Ocular trauma can also cause these infections. Corneal ulcers are usually treated with cultures to find the offending organism along with intensive regimens of antibiotic, antiviral, or antiparasitic drops to heal the infection. Treatment times for corneal infections can be as short as several days to as long as several months. In some cases, the infection can be severe enough to require a corneal transplant to restore good vision.
Learn More About Corneal Disease
Corneal Transplant Surgery
A corneal transplant is the replacement of the central portion of the cornea using donor corneal tissue (a donor graft or button) for the purpose of resorting corneal clarity, eliminating corneal swelling, improving corneal strength or thickness, or improving corneal shape.
THERE ARE THREE BASIC TYPES OF CORNEAL TRANSPLANTS:
- Anterior lamellar keratoplasty (abbreviated as: ALK, LK, or DALK) which replaces the front portion of the cornea (the stroma) without removing the innermost layer (the endothelium).
- Endothelial keratoplasty (abbreviated as: EK, DSEK, DMEK or DSAEK) which replaces only the innermost layers of the cornea and the endothelium.
- Penetrating keratoplasty (abbreviated as: PK or PKP)replacement of the full thickness of the cornea: penetrating keratoplasty.
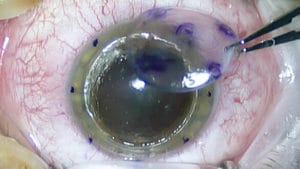
ALK
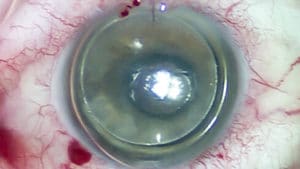
DSAEK
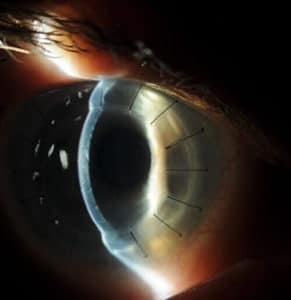
PKP
The cornea is the clear dome that covers the front surface of the eye. It is the only living tissue in the body that does not contain blood vessels. The cornea’s importance in vision is twofold: it allows light to pass into the eye, and it helps to focus that light on the retina. Therefore, a normally functioning cornea needs to be clear, thin, and the correct shape in order for light to pass through it and be bent into focus on the retina.
Corneal problems that lead to poor vision result in the cornea being cloudy (such that light is blocked), swollen (such that light is scattered), or misshapen (such that light is not focused). In addition to blurred vision, severe eye pain can result. There are numerous conditions and diseases ranging from trauma, infections, hereditary dystrophies, and previous ocular surgeries that can cause these problems.
The goal of corneal surgery is usually to restore the clear, thin and focused characteristics of the cornea. This is achieved by manipulating the existing cornea or replacing it with a corneal transplant.
Which type of corneal transplant is appropriate for you depends on your specific ocular condition. You will need to have a physical exam by your primary care physician (or the physician that best knows your health history such as a cardiologist, internist, or pediatrician) to clear you for surgery. My secretary will tell you where your surgery will be and what time to arrive. You will schedule the date of your surgery with her. If you have a problem and need to cancel or reschedule your surgery, it is very important to notify her and the surgery center as soon as possible.
You will be given a packet of information about drops and preparations for your surgery. You will be instructed not to eat or drink anything after midnight prior to your surgery. When you arrive at the surgery center, your eye will be numbed by an injection. For your comfort, you will be put to sleep for approximately 5 minutes while this injection is performed. You will then be brought into the operating room. You will be awake but drowsy. The exception to this is general anesthesia, in which you are put to sleep for the duration of the surgery. Most of the time corneal transplants are performed under local anesthesia but in some rare cases general anesthesia is necessary.
Most times the eye surgery itself lasts approximately one hour or less. Plan for the entire outpatient surgery process to last all day, and do not make plans for other activities on the same day as surgery. At the end of the surgery you will be brought to the recovery room with an eye patch in place and will be given postoperative instructions. You will need someone to drive you home after surgery.
ALK
PKP
DSAEK
DMEK
Most patients will be seen for postoperative visits according to the following schedule for penetrating keratoplasty and anterior lamellar keratoplasty:
- 1 day postoperatively
- 1 week postoperatively
- 3 weeks postoperatively
- 5 weeks postoperatively
- 2 months postoperatively
- 3 months postoperatively (half (8) of the sutures are removed)
- 5 months postoperatively (all of the sutures are removed)
- 6 months postoperatively (fitting for glasses or rigid contact lens)
For endothelial keratoplasty, on the day of surgery and on the first postoperative day, you will need to lay flat on your back as much as possible to help allow the corneal graft to attach properly.
Most patients will be seen for postoperative visits according to the following schedule for endothelial keratoplasty:
- 1 day postoperatively
- 1 week postoperatively
- 1 month postoperatively
- 2 months postoperatively
- 3 months postoperatively (fitting of glasses or rigid contact lens)
The risks of eye surgery are generally low but can include: pain, bleeding, infection, partial or total loss of vision, the need for more surgery, corneal failure, glaucoma, cataract, capsule rupture, retinal detachment, and retinal swelling. Although these problems are rare, they can occur, and you need to be aware of them before deciding to have surgery.
Donor corneas come from eye banks around the country that are regulated by the Eye Bank Association of America (EBAA). Corneas are collected from people who died and donated their corneas. The donor corneas are screened for infectious diseases and evaluated for quality and clarity. They are then refrigerated and stored in special sterile solutions. Most corneal transplant tissue is collect and used within two weeks. Poor quality corneas are not offered for transplantation unless special emergency situations arise. Donor corneas are readily available and since tissue and blood matching are not necessary, there are no waiting lists for corneas to become available.
It is common for patients to need a rigid contact lens following corneal transplant surgery. Because corneal surgery often results in an improved yet still imperfect corneal shape, this so called astigmatism is best corrected with a rigid contact lens. In some cases, glasses or soft contacts can be worn with good vision, but this is less common. It is possible, but very rare for patients not to need any type of glasses or contacts following a corneal transplant. Endothelial keratoplasties (DSAEKs, DSEKs, EKs) tend to need rigid contact lenses less often than do penetrating keratoplasties (PKPs) and anterior lamellar keratoplasties (ALKs, LPKs).
The vision after a corneal transplant depends on many factors. Some of those factors are: what was the cause of the cornea problem, how severe was the corneal disease, how is the health of the rest of the eye. Corneal transplants are usually performed to help improve the corneal shape, clarity, and or thickness. On average, the best vision following a corneal transplant comes at approximately six months after surgery (sometimes sooner, sometimes later). The target vision with glasses or a rigid contact lens is usually in the range of 20/40 (driving vision) or better. This target is variable depending on the particular case. In the first weeks to months the vision is often in the range of 20/400 (the big E on the chart). It is important to remember that frequently a rigid contact lens (rather than glasses or a soft contact lens) is required to get the best vision following corneal transplant surgery.
Corneal transplants have variable life spans depending on the type of transplant, the original reason for the transplant, the health of the patient, the health of the donor cornea, and the care the transplant receives. Some corneas last for many years and some fail requiring repeat surgery. Although every effort is made to try to insure that an eye’s first corneal transplant is also the last, some eyes end up needing more than one transplant. Endothelial keratoplasties (EK) and lamellar keratoplasties (ALK) tend to last longer and fail or reject less often. One of the best long term studies that exists regarding penetrating keratoplasty (PKP) survival comes from the Australian Corneal Graft Registry. In 2011 the study reported the survival rates of penetrating keratoplasty (PKP) for keratoconus as follows: At 10 years after surgery 89% of the transplants were still working At 20 years after surgery 49% of the transplants were still working At 23 years after surgery 17% of the transplants were still working. Archives of Ophthalmology. 2011 Jun;129(6):691-697. Epub 2011 Feb 14.
In most cases the only type of anti-rejection medications that are necessary following a corneal transplant are steroid eye drops. Some patients use these drops for several months and then stop. Some patients need to continue the steroid eye drops for the life of the transplant. Only in rare cases of frequent or very severe corneal transplant rejections are oral, systemic, anti-rejection medications necessary. It is very important if you have redness, sensitivity to light, decreased vision, or pain (“RSVP”) at any time (even years after a corneal transplant) to see an ophthalmologist immediately.
When both the cornea and the lens of an eye require surgery, whether to perform corneal transplantation first, cataract surgery first, or both at the same time is dependent on the specific situation. Only in rare cases is a corneal transplant and cataract surgery combined. This will vary depending on the patient and the status of the eye involved.